Mon - Fri 9.00 - 17.00
Call us +1 (888) 825-9321
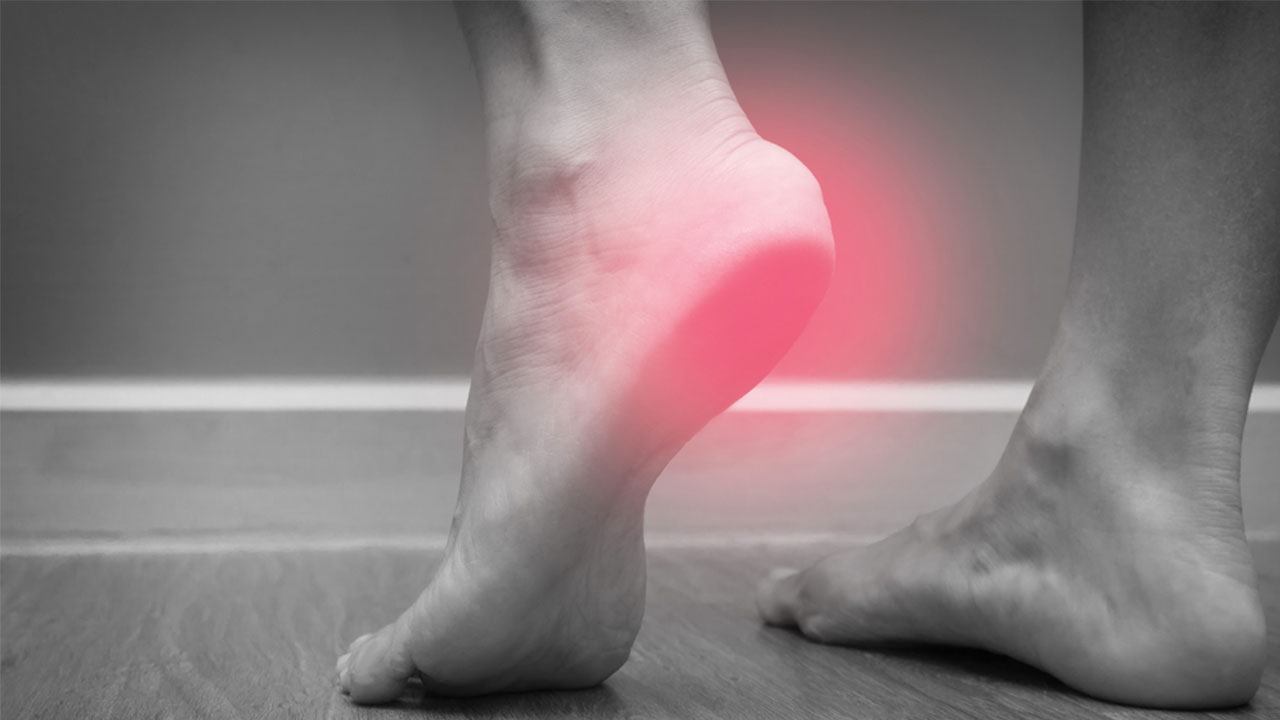
A common cause of heel pain, plantar fasciitis is an inflammation of the thick band of tissue (the plantar fascia) on the bottom of your foot, which connects your heel bone to your toes. You’ll know it by a stabbing pain right at the inner base of your heel, particularly in the morning when you first wake up after a long period of rest. Though the pain often dissipates as you move around, extended periods of standing or sitting may cause the pain to flare up again. Plantar fasciitis is most common in runners, those who are overweight, and those who wear shoes without adequate support. However, the answer to what is plantar fasciitis, what causes it and how best to treat it can sometimes be a mystery that we’ll explore below.
When the symptoms first arrive, a lot of people don’t know the cause of it. Because it’s a pain that starts in the morning and then lessens throughout the day, and because it’s often less painful while exercising than it is afterwards, it’s hard to pinpoint exactly what’s going on. Is it a sprain? A strain? Will it heal on its own? The answer is… maybe, depending on the underlying source of the issue, how severe it is, and in what state of health you are otherwise in.

The symptoms of plantar fasciitis appear gradually and then suddenly, meaning that what begins as a wince during a run and was never a cause for concern before, may result in you waking up a week later with a baffling shooting pain in your insole/heel that you don’t know how to stretch, rest, or treat. The symptoms of plantar fasciitis include:
These symptoms may cause pain, discomfort, and interruption to your normal daily activities. How did this happen to you?
Here are some general, statistically associated risk factors for developing plantar fasciitis.
This isn’t a one-size-fits-all kind of condition. The inflammation of the plantar fascia ligament occurs when it is overly strained. What causes that undo strain is the real culprit, and many factors contribute to chronic strain on the arch of the foot.
Picture the arch of your foot as a bow. The plantar fascia is the bowstring that gives you the spring in your step. It’s connected to the entire ligament, muscle, and bone system that allows you to walk upright. Consider that, and it’s easy to see how sometimes issues with the spine can cause plantar fasciitis. There is no one cause that makes for an easy answer.
Plantar fasciitis is, in essence, tissue fatigue in the foot, but it doesn’t always affect those you might expect it to. For example, while it’s common in runners, not all runners will get it, and while the obese are more vulnerable to plantar fasciitis, it truly depends on how they carry their weight more than the number represented on the scale. Much of the strain depends on how you move, and how you move is reliant on how you’re built (i.e. biological vulnerabilities), and what habits you form throughout your life to adjust to your own unique build. Let’s review some of the potential common causes of plantar fasciitis.
Bone spurs, or heel spurs, are the quickest guess when it comes to plantar fasciitis, mostly due to the fact that plantar fasciitis manifests as heel pain. However, while bone spurs are fairly common (10-20% of the population has some degree of bone spurs), and are indeed more common in those who have plantar fasciitis than those who don’t, they may not be the culprit.
This isn’t to say that bone spurs can’t be thicker, or painful, or indeed contribute to plantar fasciitis, but it is to point out that they don’t always cause tissue fatigue and inflammation. And bone spurs are certainly not the one and only cause of plantar fasciitis. Sometimes bone spurs are painless, and sometimes people with them never experience plantar fasciitis at all.
Regardless, it isn’t the spur that hurts, but the soft tissue underneath that is causing you to feel pain. Even surgically removing a spur may not take away the inflammation and injury that exists in the underlying plantar fascia (besides which, the spurs can simply grow back).
The general consensus currently is that bone spurs are incidental findings, which like wisdom teeth or the appendix exist sometimes harmlessly, sometimes uselessly, but cannot be totally counted out as either harmless or useless entirely.
Pronation is the natural motion of your foot as you walk or run. Normal pronation involves stepping down with your heel and rolling your foot slightly to the outside before shifting back to the big toe, which lifts off last from the ground as you take another step. The two ways this normal gait can go wrong in your ankle and feet are as follows.
To investigate your own gait (investigait, if you will), check the wear pattern on your shoes. If the soles of your shoes are more worn on the inner side of the heel, or the shoes tilt inwards towards each other, you’re an overpronator. If you find excess wear on the outer edges of the soles, or if the shoes when placed together tilt away from one another, you’re a supinator. Either of these can be helped with better shoe choices or by asking for advice from an orthopedist.
Adjacent to the topic of pronation is the distinction between flat feet and high arches.
Again, depending on severity, you could try correcting these issues with more appropriate footwear, targeted stretching, or by consulting with a specialist. However, if you’re here for plantar fasciitis, even if you have one of these conditions, that might not be what’s causing the problem, or it might only be a part of it. Some people have flat feet or high arches and never get plantar fasciitis. Likewise some people have pronation issues that stem instead from spinal misalignment or one one leg being longer than the other, and it’s no relation to their arches at all.
In fact, your plantar fasciitis could have nothing to do with your bones and instead everything to do with tissue and muscle tension: tight calf muscles, or Achilles tendons, or back/neck/shoulder tightness that misaligns the body all the way down. Just as the hip bone’s connected to the thigh bone, and thigh to shin, shin to ankle, so one orthopedic issue anywhere in the chain could cause a problem somewhere else.
Any and all of the above could or could not be a contributor to plantar fasciitis. That’s the tricky part of trying to treat it: if you don’t know the underlying cause, then how do you find a solution?
Most cases of plantar fasciitis can be handled at home with conservative treatments like nonsteroidal anti-inflammatory drugs (such as ibuprofen, the active ingredient in Advil and Motrin IB) or with proper stretching exercises and footwear to alleviate foot pain and guard against future strain. In other cases the condition cannot be fixed simply, and a diagnosis from a doctor may lead to professional plantar fasciitis treatment or surgery. These options may include:
If you find the symptoms of plantar fasciitis affecting the bottom of your foot, don’t let it go on so long that it becomes chronic heel pain. Do your research to find the cause or causes of the pain, and start trying the first line of treatment options at home. If the pain persists, contact an expert for advice, and follow that advice carefully so that you can avoid extreme measures, heal your connective tissue, and get back on your feet.
I need help its been a year and a half now that I have the ball of my foot is so sore and when I step on it it a hard ball and doesnt get any better. I had accupunture Lazer shock wave therapy and bought expensive ortho insoles and nothing is happening please what can I try or do next. Help.
Hi Shirley! It’s wise to always seek professional help that specialize in Plantar Fasciitis. They can help and recommend you with your therapy.
I have this problem have had 2 quarter zone injections I have inertia soles fitted in my shoes. My doctor says its a stretched day tendon but still get sharp pain in heel when bending forward .so we’re to from hear
Hi Robert! It’s always better to seek professional help that specialize on Plantar Fasciitis. Hoping on your fast recovery.
Very informative, I had plantar fasciitis and the only thing that helped me was orthopedic arch supports, I havnt had a problem since
That’s good to know, Julia. It’s really important to seek professional help on this matter. Thank you for sharing your experience, this sure will help others. 🙂
I was diagnosed with this in my right foot last year most days im ok but the days the pain is so bad i have to walk on my toes cos i cant put my right foot down to walk on.
Hi Cassandra! It is best to seek professional help that specialize in Plantar Fasciitis. They can always help us on this matter. 🙂